The 2027 Annual Update draft measure specifications are now available. Question and comment on Eligible Clinician eCQMs, Hospital - Inpatient eCQMs, and Hospital - Outpatient eCQM until December 19, 2025.
Top
Resources Subnav
Fast Healthcare Interoperability Resources (FHIR) is a Health Level Seven International® (HL7®) standard for exchanging health care information electronically. The health care community is adopting this next generation exchange framework to advance interoperability. Electronic health records (EHRs) represent patient data in different ways (e.g., medications, encounters) and FHIR provides a means for representing and sharing information among clinicians and organizations in a standard way regardless of the ways local EHRs represent or store the data. FHIR combines the best features of previous standards into a common specification, while being flexible enough to meet the needs of a wide variety of use cases within the health care ecosystem. FHIR focuses on implementation and uses the latest web technologies to aid rapid adoption.
FHIR is composed of foundational, infrastructure, administrative, data exchange, and clinical reasoning modules to support a wide variety of clinical contexts. The Clinical Reasoning Module includes a collection of resources, and operations designed to support the representation, distribution, and evaluation of clinical knowledge artifacts. These artifacts include clinical decision support rules, quality measures, public health indicators, order sets, clinical protocols, and evidence summaries. This module enables use of the same requests for information to improve care at the time of service (clinical decision support) and to evaluate care after it occurs (quality measurement), a vast improvement over previous care improvement standards.
FHIR Quality Measurement
The health care community and CMS are exploring a potential transition to FHIR-based quality measurement beginning with research and testing. Currently used quality standards, Quality Data Model (QDM), Clinical Quality Language (CQL), Health Quality Measure Format (HQMF), and Quality Reporting Document Architecture (QRDA), remain the backbone of electronic clinical quality measure (eCQM) development and reporting. However, the FHIR standard has potential to better align with the EHR's ability to share data in clinical settings, to improve alignment with clinical decision support initiatives, and to reduce overall burden on measure developers and implementers.
In order to assess the transition to FHIR quality measurement, it is important to understand the components of an eCQM and how the components will evolve with FHIR. As shown in the graphic, an eCQM is composed of three primary parts, the data model, expression logic, and structure.

- Data Model: How to describe the patient’s medical record data needed to calculate the measure
- Expression Logic: How to calculate the result and evaluate the performance
- Structure: The container and sections describing measure metadata, numerator, denominator, exclusions, exceptions
The left side of the graphic shows the current state and the right side of the graphic shows the potential future state if CMS adopts FHIR for eCQMs.
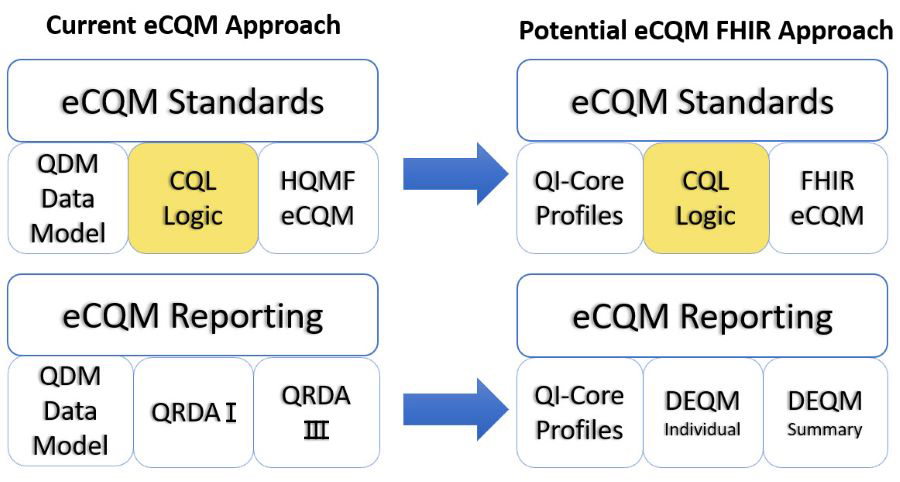
A FHIR eCQM uses the FHIR Quality Measure Implementation Guide and the Quality Improvement Core Framework (QI-Core) Implementation Guide. The goal is to align quality measurement standards for eCQM development and reporting:
- Quality Improvement Core Framework (QI-Core) replaces QDM for clinical data. QI-Core is a version-specific data model built directly on top of FHIR resources (US Core and base FHIR resources).
- FHIR Quality Measure replaces HQMF for eCQM structure. The Quality Measure IG provides guidance in using the FHIR Measure resource for eCQM structure.
- DEQM individual and summary reporting replace QRDA I and QRDA III reporting.
FHIR Resources
Resources are the basis for all exchangeable FHIR content. Each resource includes a standard definition and human-readable descriptions about how to use the resource. Each resource also has a set of common and resource-specific metadata (attributes) to allow its use clearly and unambiguously. FHIR Resources can store and/or exchange many types of clinical and administrative data, which is the foundation for the data model used in quality measurement.
FHIR Profiles and Implementation Guides for Quality Measurement
A profile is a FHIR Resource that has been changed to meet the needs of a specific use case. For example, a measure developer may use the FHIR Observation resource to indicate anything observed about a patient. To indicate vital signs, there is a requirement for a vital signs profile, which provides greater structure by listing specific data (e.g., blood pressure, respiratory rate) along with appropriate coding for the specific data element(s). Using the vital signs profile in EHRs avoids variation and makes data sharing easier.
The FHIR community often assembles multiple easily consumable profiles into implementation guides (IGs). As an example, QI-Core is an IG containing profiles for representing the clinical data in an eCQM.
For the purposes of investigating a transition to FHIR-based quality measurement, CMS is collaborating with HL7 to advance emerging standards and develop additional FHIR profiles for both eCQM development and reporting.
| Data Model | Quality Measures | Measure Reporting | |
|---|---|---|---|
| Base Resource | US Core* | Measure Resource | Measure Report |
| Implementation Guide | QI-Core | FHIR Quality Measure Implementation Guide | DEQM |
*US Core is an implementation guide representing FHIR for the US Realm
Exchange Specifications
The exchange specification defines how to exchange and manage resources in the form of real-time Representational State Transfer (RESTful) application programming interfaces (APIs) and messaging and documents. RESTful APIs allow for the exchange of FHIR resources using HTTP requests. The exchange specifications provide the foundation for reporting of eCQMs using FHIR.
Benefits of FHIR
- Provides faster, real-time access to quality data
- Reduces burden for reporting quality measures
- Aligns CMS eCQM reporting with industry clinical data exchange framework, reducing implementation burden
- Enables automated data retrieval from EHRs and submissions of quality data through use of standards-based APIs
- Promotes interoperability
- Aligns data exchange requirements for quality measurement and reporting with interoperability standards used in other health care exchange methods
- Allows for additional quality data exchange methods
- Reduces effort to implement new measures
- Simplifies data mapping to a single FHIR mapping vs. mapping to HQMF and QRDA
- Improves alignment between eCQMs and clinical decision support
- Both use a common FHIR data model (FHIR QI-Core)
Disclaimer
FHIR® is the registered trademark of HL7 and is used with the permission of HL7. Use of the FHIR trademark does not constitute endorsement of the contents of this repository by HL7, nor affirmation this data is conformant to the various applicable standards.
