Standards-based Clinical Practice Guidelines for the Digital Age
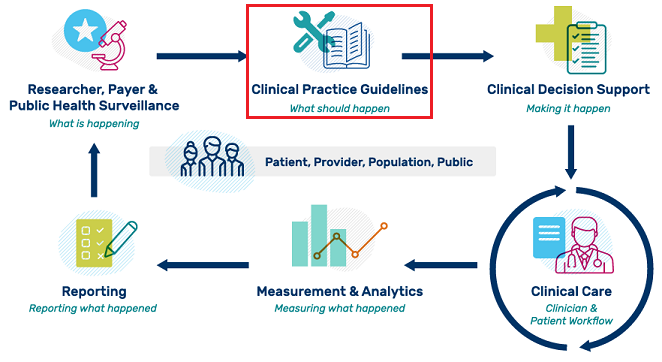 The ultimate goal of standards-based clincial practice guidelines is seamless, quick, accurate, and consistent translation and adoption of evidence-based guidelines into patient care.
The ultimate goal of standards-based clincial practice guidelines is seamless, quick, accurate, and consistent translation and adoption of evidence-based guidelines into patient care.
Automating clincial guidelines considers the implementation of computable clinical guidelines for use in Clinical Decision Support (CDS) and electronic clinical quality measures (eCQMs) during guideline development and uses Fast Healthcare Interoperability Resources® (FHIR®)-based technical standards known as CPG-on-FHIR®. “A foundational tenet of CPG-on-FHIR® approach is the concept of one faithful representation of the written guideline in computable format (i.e., the computable guideline) with many ways to implement it.”
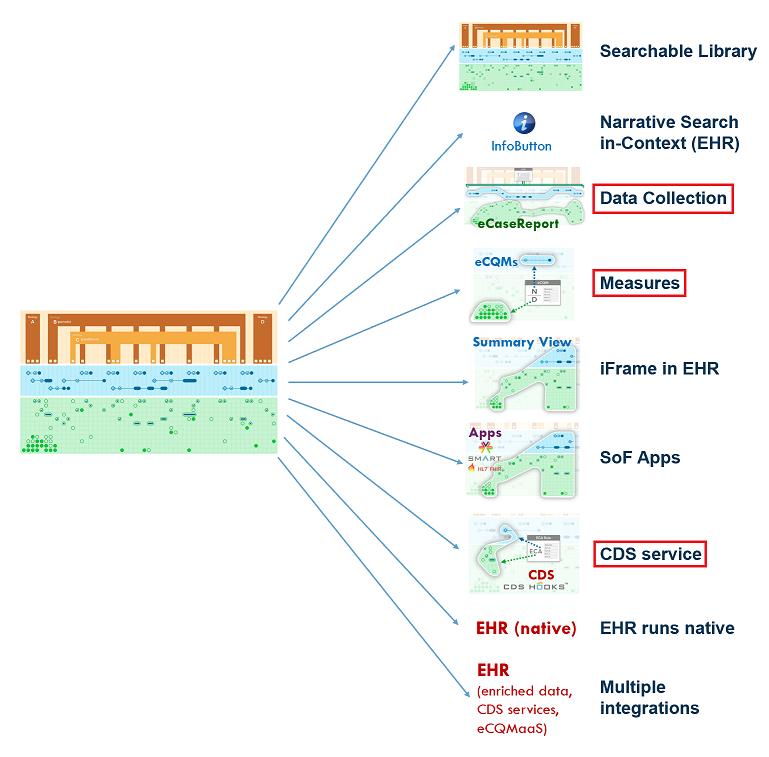
One translation
Many Ways to Implement
Adapted from: https://hl7.org/fhir/uv/cpg/documentation-approach-03-conformance-levels.html
Standards-based clinical practice guidelines provide several benefits and better ways to translate critical information into digital approaches or products including speeding up application dissemination and translation facilitation; and enhances connection with patient care.
- Fast Healthcare Interoperability Resources (FHIR) Implementation Guide
- American Journal of Medical Quality featured supplementincluding:
- Commentary:Modernizing Guidelines Development to Speed the Transfer of Science to Patient Care
- Summary of a Holistic and Multidisciplinary Approach
- An Integrated Process for Co-Developing and Implementing Written and Computable Clinical Practice Guidelines
- An Evaluation Framework for a Novel Process to Codevelop Written and Computable Guidelines
- Multi-Organizational Complex Process Redesign for Adapting Clinical Guidelines
The standards developed and used through Adapting Clinical Guidelines for the Digital Age support the clinical quality ecosystem by considering the entire learning health system. A computable guideline developed using CPG-on-FHIR® can be modularly reconfigured into multiple types of derivatives, such as CDS and eCQMs. In other words, the computable guidelines that represent a faithful translation of the evidence-based guidelines in computable form can be rearranged like Lego blocks into different ways to support patient care, such as supporting shared decision-making at the point of care through CDS or measuring patient outcomes through eCQMs.
Current standards:
